Dr Peter Yan
Gleneagles Medical Centre
The management of coronary artery disease can be divided into 2 parts. The first and very important is the primary prevention of development of coronary artery disease. The second is the definitive treatment of established coronary artery disease (secondary prevention).
1. WHAT IS MEANT BY PRIMARY PREVENTION?
Taking steps to reduce risk factors before coronary artery disease develop is called primary prevention.
Currently the expanded goals of primary prevention aim to:-
- Prevent/delay the onset of atherosclerosis (deposition of cholesterol) in the coronary arteries before it happens.
- Slow the progression of atherosclerosis in the coronary arteries (if it is present sub-clinically as confirmed by coronary CT angiogram scan).
- Stabilize cholesterol plaques in the coronary arteries so as to prevent the rupture of the plaques leading to clot with formation in the arteries thereby leading to heart attack and potential sudden death.
The prevention of coronary artery disease is simple but requires a fair amount of knowledge and discipline. It involves the modification and possible removal of the coronary risk factors which includes:-
- Cholesterol
- High blood pressure
- Diabetes mellitus
- Overweight / obesity
- Smoking
- Physical inactivity
Cholesterol control
- If a person had never had coronary artery disease, the goal is to try to achieve a blood cholesterol level of below 200 mg/dL or an LDL level (the bad cholesterol) of between 100 – 130 mg/dL.
- Once there is confirmation of coronary artery disease and especially with other added risk factors which will be discussed in the next paragraphs then the total cholesterol level should drop below 180 mg/dL and preferably below 160 mg/dL and a surrogate LDL level of below 100 mg/dL and preferably below 80 mg/dL in the very high risk groups. (Based on the Singapore Lipid guidelines)
- This can be achieved with a combination use of dietary therapy and anti-lipid drugs (eg. statins).
Dietary therapy
- Basically a healthy diet would include the following:-Consume a diet rich in vegetables and fruits, whole grains, low-fat and non-fat dairy products, legumes, fish (at least 2 times per week) and lean meat, coupled with food choices that minimize in-takes of excess energy, saturated fat, trans fat, cholesterol and salt.
- Note the importance of focusing on the overall diet quality (dietary pattern) rather than individual foods and nutrients, balancing energy intake and expenditure, engaging in regular physical activity and increasing the importance of selecting a healthy diet program when eating outside of home is of paramount importance if one’s wish is to be successful in reducing his or her blood cholesterol through diet modification.
Overweight / Obesity
- The next risk factor to modify is the weight. Obviously if one is overweight or is obese, there will be a need to reduce weight. The key to weight reduction is to reduce the number of calories taken to match the physical activity of the individual. One also needs to engage in regular physical exercise to try and burn off the excess calories and reach an ideal body weight. Aim to keep BMI (body mass index) below 23 kg/m² (healthy range 18.5 – 22.9 kg/m² – source; Health Promotion Board).
High blood pressure
- Blood pressure is another important risk factor that should be controlled to prevent coronary artery disease. Blood pressure should be kept below 130/80 mmHg and again a diet low in salt will be a good start. This couple with increased regular physical activities can reduce your blood pressure.
Diabetes Mellitus
- Aim to avoid diet high in carbohydrates and a HBA1C of 6.0%.
Smoking
- If one is smoking then one should stop smoking and also avoid the use and exposure of tobacco products.
To summarize, the American Heart Association had come up with a summary of the diet and lifestyle goals for cardiovascular disease risk reduction in 2006. See attached table. These are very good points to note and to try and achieve a heart healthy lifestyle and nutrition pattern and also would result in minimizing the development of obesity and diabetes mellitus as well as establishing life long healthy dietary habits.
|
2. DEFINITIVE TREATMENT OF CORONARY ARTERY DISEASE
The definitive treatment of established coronary artery disease would include initially cardiac medications that will improve the blood flow to the muscles of the heart and also to stabilize the cholesterol plaques within the coronary arteries.
Cardiac medications
Once again, the recommendations for primary prevention will apply as the back bone of the treatment. Then comes the use of cardiovascular medications and this will usually include the use of
- anti-platelet agents (either Aspirin or Clopidogrel) to prevent platelet adhesion (in other words to ‘thin the blood’).
- beta-blockers (to slow the heart rate thereby reducing oxygen requirement by the heart muscle)
- nitrates (to dilate the coronary arteries so as to maximize the blood flow to myocardium i.e muscles of the heart)
- statins (to achieve the targeted LDL level of below 100 mg/dL and preferably below 80 mg/dL in very high risk patients.
- ACE inhibitor or Angiotensin Receptor Blocker (ARB) (to normalize the blood pressure and confer protection to the brain, heart and kidneys by blocking the action of an adverse hormone in the blood which is called angiotensin II which when in excess, can cause high blood pressure and heart failure. It also prevents new onset diabetes mellitus).
Coronary artery bypass surgery / Angioplasty / Stent
The definitive treatment for coronary artery disease if it is shown to be severe and patient has symptomatic chest pain (angina) despite medications would be either to undergo a coronary artery bypass surgery or angioplasty / stent.
Coronary artery bypass surgery involves the use of arterial conduits (taken from the chest and/or forearm) and occasionally veins of the lower limbs to create the conduits for the bypass across the constricted or narrowed blood vessels to establish new blood supplies to the myocardium.
The less invasive procedure will be to undergo angioplasty/stents to the coronary arteries. This has become very popular as it does not involve major surgery and can be done from the groin or from the arm with just a simple injection to delivery catheters into the coronary arteries and to use balloons to pre-dilate the coronary arteries followed by the deployment of drug eluting stents to maximize the diameter of the coronary arteries and to improve the blood flow. This mode of treatment has advanced tremendously over the last 2 decades and the results are now comparable to coronary artery bypass surgery in many patients. Obviously, the decision to select coronary artery bypass surgery or angioplasty/stent will have to be decided by the cardiologist and the cardiac surgeon in consultation with the patient for the best optimal choice of therapy. Details for the procedure for angioplasty/stents have been highlighted below.
Balloon Angioplasty
In 2004 nearly 1 million percutaneous coronary intervention (PCI) procedures were performed in the United States. Angioplasty if performed by a cardiologist and a team of specialized cardiovascular nurses and technicians, usually in a special part of the hospital called the cardiac catheterization lab.
General anesthesia isn’t needed, so you are awake during the procedure. You will receive fluids and medications for relaxation and mild sedation. You will also get blood-thinning medications (antiplatelets) to reduce the risk of blood clotting, and other medications to relax your coronary arteries.
When you are comfortable, a specialist inserts a thin, flexible catheter with a deflated balloon at its tip into your arm or leg. The catheter is threaded through the artery until it reaches and passes through the blockage (see Figure 1A). At this point, the balloon is slowly inflated, flattening the plaque against the artery wall (see Figure 1B). This process widens the artery opening and allows blood flow again at a normal (or near normal) rate (see Figure 1C). If other coronary arteries are blocked, the catheter is moved, and the procedure is repeated.
Angioplasty is not a cure for CHD. About 35% to 40% of patients develop restenosis, a renarrowing of the artery, within a year following angioplasty. Two processes are thought to cause restenosis. First, when an angioplasty is performed, the artery is stretched open by a balloon.

figure1
Figure 1:
- Catheter holding a small deflated balloon on its tip is slipped over a guidewire and positioned at the blockage.
- Inflated balloon compresses the plaques against the artery wall.
- Enlarged artery opening allows blood to flow normally. After treatment, the guidewire, catheter and balloon are removed. The procedure may be repeated if the plaque build-up returns.
Afterwards, because of the elastic properties of the artery wall, the vessel renarrows, or recoils, to something close to its original size.
Second, after angioplasty a certain amount of scar tissue develops. Usually the amount of scar tissue is very small. Sometimes, however, the scar tissue can be quite thick and may obstruct the flow of blood through the artery. Restenosis is caused by the combination of vessel recoil and growth of scar tissue.
From Balloons to Stents
Stents were developed to prevent an artery from collapsing after balloon angioplasty, and have reduced the high incidence of restenosis in people undergoing the procedure. First approved in the United States in 1994, several generations of bare metal stents have been developed, with each new generation being more flexible and easier to deliver to narrowing. In fact, the insertion of a metal stent is now becoming common practice in order to hold the vessel open and maintain blood flow, reducing the incidence of both restenosis and abrupt closure of the artery.
Before undergoing a stent procedure, you should be treated with aspirin combined with clopidogrel (Plavix). Implanting a stent does not require surgery. Instead, your doctor will make a small incision in your groin or forearm and insert a catheter into the artery, similar to the balloon angioplasty procedure (see Figure 2). A specially designed balloon catheter is used to deliver the stent to the blocked area of the artery. Once there, the balloon is inflated and expands the stent, thereby squeezing the plaque against the vessel wall and widening the artery opening. After the balloon is deflated and removed, the stent remains in the artery permanently, acting like a scaffolding to hold the plaque against the artery walls and provide structural support to keep the artery open.
Conventional bare metal stents are made of various metals, but stainless steel stents are the most common. Stents come in various sizes, depending on the diameter of the artery to be treated.
Stenting, like angioplasty, is less invasive than traditional CABG surgery. It involves a shorter hospital stay – usually 1 to 2 days – and a faster recovery than surgery. However, it does have its potential risks. Also a condition called in-stent restenosis occurs in as many as 25% of patients who receive conventional bare metal stent procedure. The most common reason for in-stent restenosis is that scar tissue from uncontrolled muscle growth forms inside the stent. If in-stent restenosis occurs, patients may need to have another balloon angioplasty or stent procedure. Until recently, doctors have had few options for preventing in-stent restenosis.
Drug Eluting Stents
New status, called drug eluting stents, has been developed to help prevent restenosis. Like bare metal stents, a drug-eluting stent is a tiny metal scaffold used to prop up arteries following plaque-clearing procedures. However, a drug eluting stent is coated with a tiny amount of a drug that slowly seeps into surrounding tissue to help prevent the formation of scar tissues that can reclog a treated artery. Compared to bare metal stents, drug eluting stents significantly reduce the risk of renarrowing within the stent. Drug eluting stent trials have shown a great reduction in the formation of scar tissue and a much lower need for repeat procedures to unclog arteries.
However, drug eluting stents may not be appropriate for every patient with CHD. Potential complications include the formation of blood clots. Studies show how blood clots may be more likely with some drug eluting stents than with bare metal stents. Some people may have an allergic reaction to the drugs used in the drug eluting stent. Drug eluting stents also may not be suitable for patients who have had recent heart surgery, women who are nursing or pregnant, or patients who might not be able to tolerate antiplatelet inhibitors that need to be taken for the prescribed duration.
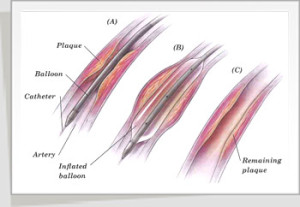
figure 2
Figure 2:
- A balloon catheter with the unexpanded stent mounted.
- Expanded stent after balloon inflation.
- Stent permanently implanted in the artery to hold the plaque against the artery wall, provide structural support to keep the artery open, and improve blood flow to the heart.
One would have to understand that the treatment of coronary artery disease is a life long treatment and cannot be stopped as the process of coronary artery disease is a progressive disease life long and has to be managed therefore on a long term basis. However once treatment has been instituted and the patient has been stabilized the lifestyle modifications and the oral medications would in most instances be sufficient to prolong the life of the patient as well as to keep the patient symptom free from angina.
Conclusion
Although improved treatment for heart disease is saving more lives, about half of all deaths occur before there is time to start treatment. Thus treatment no matter how sophisticated it may become, it is not the ideal solution of reducing deaths from heart disease. Preventing heart attacks by reducing coronary risk factors undoubtly can save lives and therefore modifying your risk factors can be thought of as preventive maintenance.